大量飲用乙醇(濫用酒精)會引發嚴重的有害後果[1]。與大量飲酒有關的健康影響(喝酒的長期影響(英語:Long-term effects of alcohol))包括會導致在酗酒、營養不良、慢性胰臟炎、酒精性肝病(簡稱為ALD)、和癌症方面的風險增加(請參考飲酒與健康)。此外,長期濫用酒精還會損害中樞神經系統和周圍神經系統。即使少量和適量的飲酒也會增加罹患某些類似癌症的風險。[2][3][4][5]
長期飲酒會損害人體的幾乎每個器官和系統。[6] 發育中的青少年的大腦特別容易受到酒精毒性的影響。[7] 此外,發育中的胎兒大腦也很脆弱,如果孕婦喝酒,可能會導致胎兒酒精綜合症(簡稱為FASD)的發生。
在西方文化中,人們在100多年前即發現飲酒與心血管疾病之間存有逆關係。[8] 許多醫生不提倡飲酒。但是,鑑於酒精相關的許多健康問題,有人建議將酒精視為一種娛樂性藥物,應該提倡透過運動和良好的營養以防止心血管疾病。[9][10] 在2013年,酒精性肝病在愛爾蘭所有慢性病的比率中,佔有五分之四。[11]
酒精相關的負面影響包括增加肝臟疾病、咽癌、食道癌、和胰臟炎的風險。相反的,適量飲酒可能對胃炎和膽結石有些益處。[12] 長期不當飲用和濫用酒精會嚴重影響身心健康。長期過量飲酒,或酒精依賴,會導致廣泛的神經精神病或神經內科系統疾病、心血管疾病、肝病、和惡性腫瘤。與酗酒有關的精神疾病包括重度抑鬱、持續性抑鬱症、人格解體、燥鬱症、輕度燥鬱症、恐慌症、恐懼症、廣泛性焦慮症、人格障礙、思覺失調、自殺、神經系統缺陷(例如工作記憶、情緒、管控功能、視覺空間能力、步態與平衡)、和腦損傷。酒精依賴與高血壓、冠狀動脈疾病和缺血性中風(ischemic stroke)、呼吸系統癌症以及消化系統癌症、肝癌、乳癌、和卵巢癌有關。大量飲酒與肝病,例如肝硬化有關。[13] 過量飲酒有加速衰老的負面影響(參考酒精對老化的影響)。[14]
一些國家推出酒類包裝警語,告知消費者有關酒精和癌症,以及孕婦飲酒會導致胎兒酒精綜合症的風險。[15]
死亡率效應
一項在2016年所做的系統評價和整合分析發現,在乙醇消費方面,與終生禁酒的人相比,適當的消費不會延長壽命。[16]在疾病對全球負擔(Global Burden of Disease)的研究數據所做的系統分析發現,乙醇的攝取會增加罹患癌症的風險,並提高全因死亡率的風險,結論是,讓疾病數量達到最小化的乙醇攝取量,是零飲用。[17]
一些研究所得的結論是,少量飲酒(在女性,飲酒少於一份,在男性,飲酒少於兩份)與「降低」心血管疾病、中風、糖尿病、和早期死亡的風險有關。[18][19] 其中一些研究把以前曾是酒精飲用者和終生禁酒者都歸為非飲酒者的一類,而把終生禁酒對健康有益的好處給遮蓋住。喝酒多過前述的少量飲酒的建議,實際上會增加罹患心血管疾病、高血壓、心房顫動、還有中風的風險[19]。暴飲可能會導致暴力或意外事故的發生,對年輕人的風險更大[19]。據信,每年約有330萬人的死亡可歸咎於酒精(佔所有死亡人數的5.9%)。[19]
建議每次最大攝入量
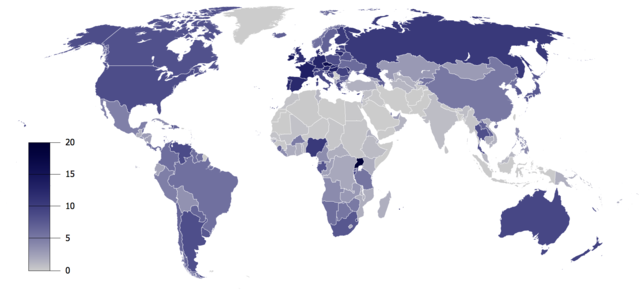
不同的國家有不同的建議最大攝入量。在英國,首席醫療官員建議男女每週喝酒不超過14單位(份)。[21][註解 1]。在大多數國家/地區,男子的建議最大數量為每週140-210公克。對於女性,範圍是每週84–140公克。(請參考各國建議攝取酒精最大數量)大多數國家建議在婦女懷孕和哺乳期間完全戒酒。
在2018年,《刺胳針》上曾發表大規模討論,但得出了互相矛盾的結果。一篇報導說"安全"飲酒的上限為每週最多7個"標準單位"的酒精飲料,相當於每週100公克純酒精。[22] 另一篇的結論是,沒有所謂安全的酒精水平,"危害健康最小化的消費水平就是不喝酒",並強調有必要在全世界修訂酒精管制政策,以減少總體的酒精消費。[17][23][24]
與酒精有關的死亡
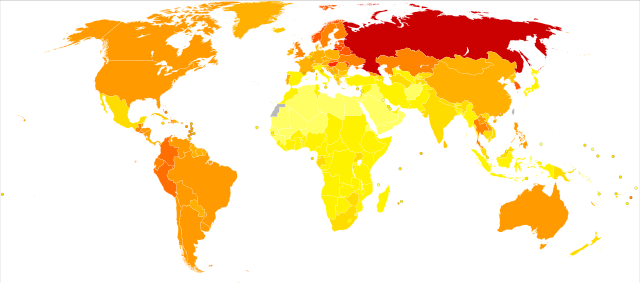
過量飲酒在世界上造成許多死亡。研究發現,飲酒導致的總死亡人數與缺乏運動的影響相似。[25] 在2009年的一項評論說,"飲酒對健康的淨影響是有害的,據估計,因飲酒而死亡佔全球所有死亡人數的3.8%,佔全球失能調整生命年(除死亡之外,還加上因為健康狀況不佳或失能而損失的『健康』年歲)的4.6%"。[26]
對西方飲酒文化的研究表明輕度至中度飲酒可能提高相關的存活率。[19][27]有一項針對12,000名,年齡在48-78歲之間的英國男性醫生進行的為期23年的前瞻性研究發現,即使把以前飲酒,但後來戒酒者併入目前的飲酒者,再和禁酒者作比較,目前飲酒者的總死亡率仍然比禁酒者低得多。這種益處在缺血性心臟病中最明顯,並在其他的血管疾病和呼吸系統疾病中也有體現。「因酒精而獲得的」疾病,如肝病和口腔癌,在飲酒者死亡率中佔比較大,而由心血管和呼吸系統疾病導致的死亡率,相比之下則不算高。每週攝取8至14個'單位'時,死亡率最低。在英國,1「單位」為10毫升或8公克純酒精。[28]
較高的攝取量會增加總死亡率,但沒有超過禁酒者的對照組。[29]其他研究發現,低度至中度飲酒所導致年齡相關的死亡風險:16-34歲的個體風險增加(由於罹患癌症、意外事故、肝病、和其他因素的風險增加),對55歲以上的人,風險則降低(由於較低的缺血性心臟病發生率)。[30]
這與其他研究所得的結論一致,研究發現中老年男性的飲酒量與總死亡率之間存在J型曲線相關性。以前飲酒,但後來戒酒者,和重度飲酒者的死亡率顯著提高,但中度飲酒者的全因死亡率可能降低15-18%。不同國家和地區之間飲酒的定義不同,但這項整合分析發現,低酒精攝取量(女性每天飲酒1-2份,男性每天2-4份)的死亡率低於禁酒的人。[31]
另一項研究[32][33]則對這種結論提出質疑,該項研究發現,在某些品質不高的研究中,把偶爾喝酒,或從前喝酒,後來戒酒的人,歸類成為禁酒的人,從而導致這一類人群的死亡率增加。但是,把上述混雜因素排除後做的研究,再次證實全因死亡率和心血管疾病死亡率(CHD mortality)會產生J型曲線。[34][35][36][37]似乎從來沒有人討論過,那些被歸類為禁酒的人中,有多少比例的人已經因慢性病而處於較高的死亡風險中,並且由於健康或與藥物會產生有害反應的原因,才不飲酒,或者不能飲酒。
觀察到的輕度至中度飲酒者,與禁酒者比較而有較低的死亡率,可能部分原因是由於飲酒者有較好的健康狀況和較高的社會地位所致;[38] 然而,即使把這些混雜因素調整之後,飲酒對於輕度至中度飲酒者提所供的保護作用仍然顯著。[35][37]此外,類似少報酒精攝取量等混雜因素,可能會導致把輕度至中度飲酒者的死亡率低估。[34][39]
在2010年所做的一項研究,證實適度飲酒對死亡率有好的影響。[37]將受測試者分為禁酒者、輕度、中度、和重度飲酒者。死亡率從最低到最高的順序為中度、輕度、重度、和禁酒者。禁酒者的死亡率風險增加是中度飲酒者的兩倍。這項研究專門尋求控制那些混雜因素,包括把以前飲酒,但後來戒酒者被視為非飲酒者的問題。[37]根據另一項研究,酒精攝取量大的飲酒者(一次喝六份或更多),比飲酒攝取量小的人,全因死亡率高出57%。[40] 年輕的禁酒者死亡率最低,年輕的重度飲酒者死亡率最高。[41]
根據2018年的一項研究,每週喝酒超過7份標準量,最多喝到14份標準量的人,預期壽命可能會縮短6個月左右。那些每週喝酒超過14份且最多喝到25份的人,其預期壽命可能會縮短1-2年,而每週喝酒超過25份的,則會縮短4-5年。[22]
與西方文化的研究相比較,在其他文化中的研究則得到相反的結果。著名的INTERHEART Study所做的研究,南亞人的飲酒並不能預防心血管疾病,和其他地區人口因喝酒而有益處的結果有鮮明的對比。[42]實際上,飲酒的亞洲印度人在心臟病發作的風險高出60%(其中喝本地烈酒的佔80%,而喝有品牌烈酒的佔50%)。[43]在歸類為偶爾,和經常的輕度、中度、和重度飲酒者中都發現有這種危害。[43]
在印度,針對4,465名受測試者所進行的另一項大型研究也證實,飲酒會產生對男性心血管疾病的危害。與禁酒者相比,飲酒者的血糖高出2mg/dl(2毫克/公升),血壓高出2mmHg(2毫米汞柱),和高密度脂蛋白膽固醇高出(2mg/dl)(2毫克/公升),這類人吸煙的比率也比禁酒的人高得多(63%比21%)。[43]
一項研究聲稱,"近年來,俄羅斯人過度飲酒,尤其是男性,佔年齡層在15-54歲之間死亡人數的一半以上。"[44] 但是,這項研究存有一些難題。例如,同一項研究還發現大量飲酒對乳癌死亡率具有保護作用。這與公認的科學觀點相矛盾,即酒精會增加罹患乳癌的風險。[45] 關於這一點,在做進一步溝通討論之後,得到的建議是"需要對與飲酒有關的死亡率統計數據做仔細的解讀,同時要考慮到其他相關的危險因素、發病率、和存活率。"[46]
在英國的一份政府報告中的資料,"在2007年與酒精有關的死亡人數是8,724人,比2006年要低,但比1991年記錄的4,144人增加兩倍多。與酒精有關的死亡率在2007年為每10萬人中有13.3人,1991年每10萬人中有6.9人。" [47] 在蘇格蘭,國民保健署估計在2003年每20人中就有1人的死亡與酒精有關聯。[48] 2009年的一份報告指出,與酒精有關的疾病所導致的死亡為9,000人,是25年前的3倍。[49]
英國的一份報告得出的結論是,低度至中度飲酒對死亡率的影響取決於年齡。低度至中度飲酒會增加16-34歲間個人的死亡風險(由於罹患癌症、意外事故、肝病、和其他因素的風險增加),但會降低55歲以上個人的死亡風險(由於缺血性心臟病的風險降低的緣故)。[50] 英國的一項研究發現,酒精在英國所引起的癌症約佔全部癌症病例的4%(每年12,500例)。[51]
美國疾病管制與預防中心(簡稱為CDC)報告:"從 2001年至2005年,每年大約有79,000人死於過量飲酒。事實上,過量飲酒是美國人每年與生活方式相關的第三大死亡原因。"[52]在1993年的一項研究估計,美國因飲酒而死亡的人數為100,000。[53]
CDC在2001年的另一份報告估計,當年在美國,中度和高度飲酒導致75,754人死亡。飲酒量低有一些有益的作用,因此,淨死於酒精的人數是59,180人。[54]
壽命
2016年,有項飲酒和死亡風險研究,針對87項案例做整合分析。案例分析後的結果,中度飲酒者死亡率風險降低的最大,但這些研究並未糾正某些定義為禁酒者相關的混淆變數,例如這些人是否有先前的酗酒和慢性健康上的問題。在對這些針對禁酒者變異做調整之後,發現小量飲酒者的死亡率沒有降低。[55]然而,另有個別研究顯示,對55歲以上的人進行混雜因素調整後,禁酒者和重度飲酒者的死亡率比中度飲酒者的增加約50%。[56]
心血管系統
酒精具有抗凝血作用。[57]中度飲酒者的血栓形成率比禁酒者低。[58]一項對隨機試驗的整合分析發現,適度飲酒會降低血清纖維蛋白原(一種促進血凝塊形成的蛋白質)的水平,同時會增加組織型纖維蛋白溶酶原激活物(一種有助於溶解血凝塊的酶)的水平。[59]估計這些變化可將冠狀動脈疾病風險降低約24%。2011年的另一項整合分析發現,中度飲酒,會對有關的高密度脂蛋白膽固醇、脂聯素、和纖維蛋白原發生有利變化。[60]
根據針對16,351名參與者的系統評價顯示,心血管疾病死亡率與飲酒量之間的總體關係以J形曲線呈現。每天飲酒5-10公克有最大的保護作用,到每天飲酒26公克時仍然效果顯著。[61]中度飲酒者的血清C反應蛋白(簡稱為CRP)是炎症和心血管疾病風險的預測指標,其水平低於禁酒者,這表明適度飲酒可能具有抗炎症作用。[62][63][64]一項前瞻性研究的數據顯示,在最初飲酒量較低(每週喝酒少於或等於1份的男性)者中,隨後適度增加飲酒量,可能會降低他們在心血管疾病的風險。[65]
雖然是有前面說的流行病學上的證據,許多人還是提出不要為了健康而飲酒的建議。世界衛生組織(簡稱為WHO)的一名醫生將這種提倡飲酒的行為標誌為"荒謬而危險的"。[66][67]一位評論者指出:"儘管有豐富的觀察數據,但因為尚未進行任何隨機對照試驗,尚無絕對明確的證據表明酒精可降低心血管疾病的風險。不應該建議患者使用酒精去降低心血管疾病的風險,來替代那些已經被充分證實過的方法:如適當的飲食、運動、和藥物等。」 [68]
有人認為,酒精對健康的好處,縱然說有,但還有爭議,而且酒類產業可能把這一觀點加以擴大,研究人員認為,酒精應被視為是對健康有潛在嚴重不利影響的娛樂性藥物,不應推廣用來對心血管疾病提供保護。[69][70]
在1997年發表的一項前瞻性研究發現,"適度飲酒似乎可以降低看來明顯健康的男性罹患周邊動脈疾病的風險。"[71]在一項針對人群的大型研究的結果顯示,適度飲酒與女性罹患周邊動脈疾病成反比,而與男性則無這種現象。但是,當把吸煙這種混淆因素列入考慮時,這種好處就擴展到了男性。這項研究得出的結論是"在不吸煙的男女中,飲酒與周圍動脈疾病之間存在負相關的關係。" [72][73]
有一項研究發現,適量飲酒對間歇性跛行有保護作用。對每天喝1至2份酒的男性,和每天喝半份至1份酒的女性,風險最低。[74]
適量飲酒經發現可幫助心臟病發作的人存活。[75][76][77]但是,過量飲酒會增加心臟衰竭的風險。[78]文獻評論說,半份酒精飲料提供的保護水平最佳。但是他們指出,目前尚無隨機對照試驗來證實低劑量酒精對心臟病發作具有保護作用。[79]如果每天服用3份或更多的標準量酒精飲料,則會增加高三酸甘油脂血症、心肌症、高血壓、和中風的風險。[80]一項系統評價報告說,依照劑量方式來減少重度飲酒者的攝取量,可降低血壓。對於每天喝兩份或更少酒的人,則沒有發現有差異。[81]
長期攝取大量的酒精會導致酒精性心肌症。酒精性心肌症的臨床症狀與病因不明擴張型心肌病相同,涉及心臟肌肉組織肥大,可導致心臟衰竭。[82]
神經系統

長期大量飲酒會損害大腦發育,導致酒精相關性失智、腦損傷、身體依賴、酒精性周邊神經病變(也稱為「酒精腿」,alcohol leg),加劇神經精神方面和認知的障礙,並導致神經化學異常。目前,由於不良的研究設計和方法,關於適度飲酒會增加還是降低失智症的風險,尚無文獻給予定論。[85]一些研究提出,低度至中度飲酒對年齡相關的認知能力下降,以及失智症有保護作用。然而,其他研究尚未發現低度至中度飲酒有這種保護作用。[86]
一些證據顯示,低度至中度飲酒可能會加速大腦容量的損失。[87]長期飲酒可能導致血漿中有毒氨基酸高半胱氨酸水平升高,[88][89]這可能是酒精戒斷症候群發作的原因,[90]酒精引起的腦萎縮[91],以及與酒精相關的認知障礙[92]。酒精對神經系統的影響還包括記憶力和學習障礙(請參閱酒精對記憶的影響),例如導致失憶症現象。
針對中年人群所做的流行病學研究,通常發現飲酒與中風風險之間的關係呈U型或J型曲線的形式。[93][94][95][96] 根據所研究的中風類型,酒精可能會有很不同的影響。在西方文化中,中風的主要形式是缺血性,而在非西方文化中,出血性中風案例則較多。,每天攝入2份以上的酒精飲料與酒精對缺血性中風的有益作用相反,會增加出血性中風的風險。
美國國家中風協會估計,大量酒精攝取酒精會讓中風的風險增加50%。[97]"對於中風,在特定人群中觀察到的飲酒與危險之間的關係,取決於出血性中風的比例。輕度至中度飲酒可降低缺血性中風的風險,這在一定程度上可能有因果關係。另一方面,出血性中風與飲酒呈對數線性關係。"[98]
酗酒與廣泛而嚴重的大腦損傷有關。與酒精有關的腦部損傷不僅是由於酒精的直接毒性作用所致;而且酒精戒斷症候群、營養不良、電解質紊亂、和肝損傷等,也被認為會導致與酒精有關的腦部損傷。[99]
過量飲酒與前瞻性記憶受損有關。這種認知能力的受損,導致日後無法執行未來該做事情的狀況會增加,例如,忘記鎖門或按時寄信。所攝取的酒精量越高,飲用的時間越長,損害就越嚴重。[100]對長期飲酒的毒性最敏感的器官之一是大腦。在美國,大約20%的精神病院的入院,都與酒精相關的認知障礙有關,最明顯的是酒精相關的失智症。
長期過量飲酒還與嚴重的認知能力下降,和一系列神經精神科併發症有關。老年人在酒精毒性對大腦的作用最敏感。[101]有一些不確定的證據顯示,在成年早期攝取少量酒精,對以後的生活具有保護作用,可防止認知能力下降和失智。[102]然而,一項研究得出的結論是:"我們的發現表明,儘管有先前的建議,但適度飲酒並不能保護老年人免受認知能力下降的影響。"[103]
魏尼克-高沙可夫症候群是維他命B1缺乏的一種表現,通常是酗酒的副作用。[104]該症候群是兩種同名疾病的綜合表現,即高沙可夫症候群和魏尼克腦病。魏尼克腦病的表現是急性的,其特徵是意識模糊,而高沙可夫症候群的主要症狀是失憶症和管控功能障礙。[105] 香蕉袋是裝有維生素和礦物質(由於維生素而呈亮黃色)的靜脈注射液容器,可用於減輕這些後果。[106][107]
通過喝少量的酒精可對原發性顫抖症患者,或者在有原發性顫抖症家族史的背景下,可在發生後短暫緩解患者多達三分之二的症狀。[108]
已知乙醇會激活A型γ-氨基丁酸受體(簡稱為GABAAR)並抑制N-甲基-D-天門冬胺酸受體(簡稱為NMDA),這些均與原發性顫抖病理有關[109] ,並且可能是改善作用的基礎。[110][111] 另外,在不同的動物原發性顫抖症模型中,也做過乙醇作用的研究。(有關此主題的更多詳細信息,請參閱「原發性顫抖症」的英文版。)
長期使用酒精來引導睡眠會導致失眠:在睡眠階段之間頻繁變動,會因頭痛和流汗而醒來。停止長期酗酒還會導致夢境生動,嚴重影響睡眠。長期酒精濫用與非快速動眼睡眠第3和4期,以及抑制快速動眼期睡眠,還有快速動眼期睡眠破碎有關。在酒精戒斷症候群期間,快速動眼期睡眠的發生,通常被放大稱為是快速動眼期睡眠反彈作用的一部分。[112]
大量飲酒者和酗酒者發生嚴重抑鬱症的概率很高。雖有某些證據表明飲酒會導致這種嚴重抑鬱疾病,但是否由抑鬱症導致自我用藥酒精濫用,還是飲酒引起的酗酒者抑鬱症增加,還未有定論。[113]酗酒與許多精神健康疾病相關,同時酗酒者的自殺率很高。[114]一項針對因自殺未遂而住院的人所做的研究顯示,酗酒者後續成功自殺的可能性是非酗酒者的75倍。[115]在一般酗酒者人群中,自殺風險比普通人群高5-20倍。大約有15%的酗酒者會自殺。濫用其他藥物也會增加自殺的風險。35歲以下的年輕人中約有33%的自殺與酒精或其他物質濫用有關。[116]
由於酒精對大腦,尤其是大腦前額葉皮質區的神經毒性作用,在酗酒的人中社交技能顯著受損。受到酗酒損害的社交技能,包括面部表情感知能力、語言韻律感知能力、和心智理論感知能力;酗酒者也無法理解幽默。[117]
研究結果顯示,酒精依賴與酒精戒斷後的渴望 和易怒直接相關。[118]另一項研究顯示,飲酒是導致兒童反社會行為的重要誘因。[119]憂鬱症、焦慮症、和恐慌症是酒精依賴者通常罹患的疾病。酗酒與負責處理情緒的大腦網絡(例如杏仁核和海馬體)的活化減弱有關。[120]長期戒酒之後,精神健康障礙症狀的改善或消失,表示這種障礙通常是由於酒精濫用引起的大腦神經化學畸變而引起的,但這障礙問題在戒斷初期和恢復期間可能會有惡化的情形。[121][122][123] 思覺失調會發生在幾種酒精相關疾病之後,包括急性中毒和大量爛飲之後的戒斷時期。[124]與其他濫用藥物相比,長期濫用酒精更會導致思覺失調症狀的發展。已有證據顯示,酗酒會導致男性思覺失調的風險增加800%,女性思覺失調的風險增加300%,而這與先前存在的思覺失調疾病並無關聯。這明顯高於因使用大麻所產生的結果,讓酗酒成為導致思覺失調的非常重大原因。[124]約有3%的酒精依賴者在急性中毒或戒斷期間會出現思覺失調的情況。與酒精有關的思覺失調可能會透過藥物戒斷併發引發機制展現出來。與酒精有關的思覺失調的機制是由於神經元膜變形、基因表現、以及維他命B1缺乏所致。在某些情況下,酗酒,會透過藥物戒斷併發引發機制,可能會導致慢性藥物引發的精神病(即精神分裂症)的發展。與酒精有關的思覺失調的影響包括抑鬱和自殺,以及社會心理障礙的風險增加。[124]然而適度的飲酒,顯示是可降低罹患抑鬱症的風險。[125]
雖然酒精最初會幫助克服社交恐懼症或恐慌症狀,但長期濫用酒精經常會加重社交恐懼症的症狀,並在酒精中毒期間,尤其是在酒精戒斷症候群期間,會導致恐慌症的發展或惡化。這種作用並非只是酒精所獨有,但長期使用與酒精具有類似作用的藥物(例如苯二氮䓬類藥物)也可能發生,苯二氮䓬類藥物有時被開立處方,作為有酒精問題的人服用的鎮靜劑。[126]約有一半因精神焦慮症(如恐慌症或社交恐懼症)而接受精神醫療服務的患者,患有酒精依賴,或苯二氮䓬類藥物依賴的問題。應當指出,每個人對酒精或鎮定劑,安眠藥都有各自的敏感性水平,一個人可忍受而不會生病,而另一個人則會因同樣原因而生大病,並且即使只有適度飲酒也會引起反復性症候症和睡眠障礙。遭受酒精毒害的人,將無法從其他療法或藥物中受益,因為它們的根本原因並未解決。[127]
酒精成癮與迄今為止的任何藥物濫用所測試出來的結果都一樣,與伏隔核中GLT1(EAAT2)的持續下降有關,並且與所有文獻記錄裏的成癮綜合症中,幾乎千篇一律的覓藥行為(drug-seeking behavior)有關。麩胺酸傳遞的長期失調、加上與重新暴露於藥物使用而觸動情況復發、以及對其他改善藥物成癮的可能性的總體增加,讓情況更為不利。目前已有有助於重新穩定穀氨酸系統的藥物,例如乙酰半胱氨酸,用於治療對可卡因,尼古丁,和酒精成癮的症狀。[128]
消化系統和體重增加
酒精對體重增加的影響是有爭議的:一些研究沒發現有這樣的效果[129],另一些研究則發現對體重有減少[130]或者增加的影響。
在美國進行的一項國民健康與營養檢定調查(NHANES)得出的結論是:"輕度至中度飲酒與代謝症候群的患病率較低有關,對脂肪、腰圍、和空腹胰島素產生有利影響。這種關係在白人中,以及喝啤酒及葡萄酒的人最為明顯。[132]同樣,在韓國進行的一項全國調查顯示,酒精攝取與代謝症候群之間存在J形曲線關聯:"本研究的結果顯示,代謝症候群與輕度飲酒呈負相關(韓國成年人每天飲酒1–15公克)",但在飲酒量大的人,則危險會增加。[133]
研究發現,飲酒可降低膽結石的發生風險。根據年齡、性別、教育程度、吸煙與否、和身高體重指數來分類,和禁酒者做比較,偶爾和經常輕度飲酒者(每天少於25公撮)的膽結石相對風險為0.83,中度飲酒者(每天25-50公撮)為0.67,重度飲酒者為0.58。這種反向關聯在年齡、性別、和身高體重指數的各個層次上都是一致。[134]飲酒頻率似乎也是一個因素。"飲酒頻率的增加也與降低風險有關。結合飲酒量和飲酒頻率的報告,反映出任何給定飲酒量(5-7天/週)的頻繁攝取的方式與不飲酒者相比,患病風險降低。相比之下,不經常飲酒(1-2天/週)與患病風險沒有顯著相關性。」 [135]
在1998年發表的一項大型自我報告研究發現,膽囊疾病與多種因素(包括吸煙、飲酒、高血壓、和喝咖啡)之間沒有關聯。[136]在1997年所做的一項回溯性研究發現,在飲酒者中使用維生素C(L-抗壞血酸)補充劑與膽囊疾病的患病率較低相關,但在非飲酒者中未發現有這種關聯。[137]
酒精性肝病是一種主要的公共衛生問題。例如,在美國有多達200萬人患有與酒精有關的肝病。[138]長期酗酒會導致脂肪肝、肝硬化、和酒精性肝炎。治療選擇有限,最重要的就是停止飲酒。碰到嚴重的肝病,唯一的治療選擇可能是來自禁酒者捐贈的肝臟移植。目前正在研究腫瘤壞死因子抑制劑的有效性。某些補充藥物,例如水飛薊和水飛薊素,似乎可提供一些效果。[138][139] 酒精是西方世界中導致肝癌的主要原因,佔肝癌病例中的32-45%。在美國有多達50萬人罹患有與酒精有關的肝癌。[140][141]
酗酒是導致急性胰臟炎和慢性胰臟炎的主要原因。[142][143]酒精性胰臟炎可產生嚴重的腹痛,並可能發展為胰臟癌。[144]慢性胰臟炎通常會導致腸道吸收不良,並導致糖尿病。[145]
酒精會影響長期飲酒者的營養狀況。它會減少食物攝取並導致吸收不良。它會導致骨骼肌質量失衡,並導致肌肉萎縮。長期飲酒還會增加人體中重要蛋白質的分解,從而影響基因表現。[146]
其他系統
長期攝取酒精會損害肺部的多種關鍵細胞功能。[147]這些細胞損傷可導致因肺部疾病,嚴重併發症發生的可能性。最近的研究指出,與酗酒導致的肺部疾病相關的死亡,與酒精導致肝病的死亡可相提並論[148],與禁酒者比較,酗酒者罹患急性呼吸窘迫症候群(簡稱為ARDS)的風險,與因為ARDS而死亡的比率較高[149]。一項大規模的前瞻性研究與這些發現相反,認為適度飲酒對呼吸道疾病導致的死亡具有保護作用。[29]
長期過量飲酒會導致中樞神經系統和周圍神經系統受損,導致男性性慾減退和陽痿。[154]這是由於乙醇引起的睾丸萎縮,導致睾丸激素分泌減少,男性的女性化程度提高,也是酗酒男性肝硬化的臨床特徵。[155]
過量飲酒會導致雌激素過多。[156] 據推測,含酒精的飲料可能含有類似雌激素的化合物。在男性中,高水平的雌激素可導致睾丸功能衰竭,和發展出女性特徵,包括男性乳房的發育(男性乳房發育症)。[157][158] 在女性中,由於過量飲酒會導致雌激素水平升高,與乳癌風險增加有關。[158][159]
一項整合分析,以終生禁酒者為參照群,透過性別和指標(end point)來確定劑量-反應之間的關係。分析發現,對於男女兩性都呈現U形曲線的關係。與終生禁酒者相比,男性中2型糖尿病的相對風險(簡稱為RR)在每天飲酒22公克時保護作用最高,而每天飲酒60公克以上時有害。在婦女中,每天飲酒24公克時保護作用最高,每天飲酒約50公克時變得有害。[來源請求]對婦女干預研究的系統評價,所得結果也支持這項發現。報告說,適度飲酒可提高女性的胰島素敏感性。[160]
飲酒的方式(即進餐時飲用,或是暴飲)會影響各種健康結果[161]。可能的情況是,與大量飲酒有關的糖尿病風險,是由於飲酒主要是在週末一次喝完,而不是在一週內把與前述相同數量的酒分開而平均飲用所引起。[161] 在英國針對暴飲,會"建議避免每週飲用(暴飲)"。[來源請求]來自芬蘭的一項為期二十年的相同研究報告顯示,適度飲酒可降低男女患2型糖尿病的風險。然而,暴飲和高量飲酒會增加女性2型糖尿病的風險。[162]
經常飲酒與痛風性關節炎風險增加[163][164],和類風濕關節炎風險降低有關。[165][166][167][168][169]最近的兩項研究報告說,飲酒越多,罹患類風濕關節炎的風險越低。在經常喝酒的人裏面,其中四分之一喝酒最多的人,患病率要比喝酒最少的一半的人,發病機會降低50%。[170]
研究人員指出,適度飲酒還可降低其他發炎(如心血管疾病)的風險。乙醇可通過某些生物學機制降低破壞性關節炎的風險,並防止骨質密度(bone mineral density,BMD)的流失,而骨質密度流失是疾病發展過程的一部分。[171]
一項研究得出的結論是:"或者酒精會預防類風濕關節炎(簡稱為RA),或者患有RA的受試者會在RA發病後減少飲酒。" [172] 另一項研究發現,"更年期後婦女,平均每週喝酒超過14份的,患類風濕關節炎的風險降低……" [173]
適度飲酒與更年期後的婦女較高的骨質密度有關。 "……飲酒顯著把骨質疏鬆症的可能性降低。" [174] "更年期後年長婦女的適度飲酒與較高的骨質相關。" [175] "[45歲以上]男性和女性的社交飲酒,與較高的骨質密度相關。"[176] 但是,酗酒與骨質流失有關。[177][178]
長期過度飲酒會導致多種皮膚疾病,包括蕁麻疹、緩發性皮膚病變紫質症、潮紅、肝硬化的皮膚瘢痕、牛皮癬、癢、脂溢性皮炎、和酒糟鼻。[179] 一項在2010年所作的研究得出結論:"喝淡啤酒與女性罹患牛皮癬的風險增加有關。在這項研究中,其他酒精飲料並未增加牛皮癬的風險。" [180]
免疫系統
飲酒可預防主動感染幽門螺桿菌[181]。相比之下,飲酒(每天飲酒超過30公克的人,與不飲酒的人相比)與十二指腸潰瘍(請參考胃及十二指腸潰瘍)的較高風險無關。[182]酗酒者的過量飲酒是已知的肺炎危險因子。
一項關於普通感冒的研究發現,"大量的酒精飲料(每天最多3到4份)與感冒的風險降低相關,因為飲酒與感染後的生病減少相關。但是,飲酒的好處僅發生在非吸煙者身上。[........]雖然飲酒並沒有影響吸煙者患臨床疾病的風險,但適度飲酒會降低不吸煙者的風險。"[183]
另一項研究的結論是:"研究結果顯示,攝取葡萄酒,尤其是紅酒,可能對普通感冒有保護作用。啤酒、烈酒、和酒精攝取總量似乎並不影響到普通感冒的發生。」[183]
癌症
1988年,WHO的國際癌症研究機構把酒精列為一類致癌物,這個機構說:"有充分的證據證明酒精性飲料對人體的致癌性……酒精性飲料對人類具有致癌性(第1類)。" [184] 美國衛生與公共服務部的國家毒理學計劃在2000年把酒精列為「已知的致癌物質」。[185]
據估計,2006年"全世界中有3.6%的癌症病例與飲酒有關,因此導致的死亡佔所有癌症死亡的3.5%。" [186]在2011年所做的一項歐洲研究發現,男性癌症的10分之1,與女性癌症的33分之1,是由於過去或現在的酒精攝取所引起。[187][188]世界癌症研究基金會小組的報告《「食物、營養、體育活動、和癌症預防:全球視野」》發現 "有說服力"的證據,顯示酒精飲料會增加以下癌症的風險:嘴巴、咽和喉、食道、大腸癌(男性)、乳癌(更年期前後)。[189]
即使少量和中度飲酒也會增加個人的癌症風險,尤其是在食道鱗狀細胞癌(請參考食道癌的英文版)、口咽癌、和乳癌。[190][191]
乙醛是酒精的代謝產物,被懷疑會導致癌症。[192]通常,肝臟會把飲酒所產生的乙醛消除掉99%。但是,肝臟疾病和某些遺傳酶缺乏症會導致乙醛水平升高。已發現在重度飲酒者,由於酒精醇脫氫酶的遺傳缺陷,而暴露在高乙醛水平,罹患上消化道和肝臟癌症的風險更大。[193]在2007年所做的一項審查發現"有說服力的證據表明,乙醛...讓乙醇發生致癌作用,是由於乙醛對去氧核糖核酸(DNA)的多種促使突變作用。" [194]乙醛可與DNA反應生成包括Cr-PdG在內的DNA加合物。這種Cr-PdG加合物"可能在酒精飲料相關的致癌機制中發揮重要作用。"[195]
酒精對胎兒的影響
胎兒酒精綜合症(即胎兒酒精譜系障礙,或稱FAS,Fetal alcohol syndrome)是先天性障礙,發生在懷孕期間飲酒的婦女後代中。根據對當前知識的調查,懷孕婦女飲酒風險多於收益。[196]酒精會穿過胎盤屏障,阻礙胎兒的成長或體重,造成獨特的面部瘢痕,損害神經元和大腦結構,並引起其他身體、精神、或行為問題。[197]
胎兒接觸酒精是西方世界裏面,導致智力障礙的主要原因。[198]懷孕期間飲酒,與腦胰島素抗性和類胰島素抗性的生長因素有關。[177]
酗酒對家庭和兒童的長期影響
在酗酒家庭中長大的孩子,在涉入自己的固定情感關係時,有可能會遭受情緒上的困擾。這種孩子在離婚和分居、婚姻狀況不穩定、和家庭破裂方面,有較高的風險。[199]兒童時期經歷的抑鬱和反社會行為的情緒,經常導致婚姻衝突和家庭暴力。婦女比男子更有可能成為與酒精有關的家庭暴力的受害者。[200][201][202][203]
酗酒者的子女,經常將從孩子時期中學到的行為,納入他們自己的婚姻關係中。這些行為導致不良的養育做法。例如,酗酒者的孩子成年後,可能同時會對孩子或配偶表達愛和擯棄。這稱為不安全型依附(insecure attachment,請參考依附理論中安全型依附)。[199][202][203]不安全型依附會導致與親密伴侶和後代在信任和聯繫上發生問題。此外,先前的父母缺乏情感上的支持,會導致子女長大後,在成人關係中,缺乏解決衝突的技能。[199]證據顯示,酗酒的父親表現出苛刻和無效的養育做法,與青少年和成年人的酒精依賴有關。 [202][203]
酗酒者的子女由於害怕被遺棄而常常無法信任其他成年人。[199] 此外,由於孩子們通過觀看父母的互動來學習他們的交往行為,因此,有酗酒父親的女兒成年後可能無法與男人適當地互動。[199]酗酒父母的不良行為榜樣導致對如何進行異性互動的認識不足。[199]
酗酒者的兒子面臨自我調節不良的風險,這種情況經常在學齡前就表現出來。這導致他們將自己行為的問題,和無法控制衝動都歸咎於他人。不良的決策,特別是在酗酒者的兒子中,與他們早期就開始飲酒有關。[200][201][203]兒子經常表現出尋求刺激的行為,避免受傷害,並且表現出忍受挫敗能力不足的情況。[201][202][203]
健康風險和飲酒
有許多短期和長期的健康狀況可歸因於飲酒。有完整的記錄顯示,長期讓自己處在有害狀況下,其中一些狀況會讓幾個重要器官永久受損,很難治療。在這些情況中,來自一種或多種因素,最終的結果就是造成死亡。據報告,在2006年至2010年之間,由於過度飲酒在美國有88,000人因此死亡。[204]
醫生通常認為飲酒是讓幾種慢性病變得更難治療的直接原因,因此建議少次,少量飲酒,以防止進一步讓破壞性損害發生。一些醫生強烈建議戒酒,以預防心臟病、腦損傷、和肝病。
性功能 眾人皆知長期使用酒精會損害神經系統、心臟、肝臟、和生殖器官,導致成年男性性能力下降。此外,由於有長期飲酒精相關的精神障礙,可能會導致傾向進行無保護的性行為,和與多伴侶的性行為。這情況可能會導致曝露在性傳染病的風險,以及意外懷孕。[205]
對胎兒的影響 在懷孕期間仍繼續飲酒的婦女,極有可能生下有缺陷的後代。由於酒精能夠透過母親傳遞給嬰兒的營養,直接傳到胎盤,因此對胎兒的發育直接發生影響,導致細胞受損、先天缺陷、神經系統疾病、還有流產。[206]
對重要器官的影響 研究結果顯示,大量飲酒與器官損害之間存在着破壞性關係。心血管的問題,如高血壓、心肌病、和心臟病等,可歸因於過量飲酒。除循環系統之外,腎臟和肝臟疾病也可歸因於飲酒。也有對大腦功能的影響,例如記憶力減退而降低智力,大腦容量和協調能力的損失。[207]
社交能力影響 長期過度使用酒精會導致許多難以治療的狀況,例如抑鬱、衝動性決策、暴力、虐待行為、和認知能力下降。所有這些都會降低與家人,朋友互動的品質,並可能會導致對自己和他人做出有害的行為。[208]
長期飲酒對經濟的影響
當前沒有一致的方法來衡量飲酒在經濟上的影響。[209]疾病的直接、間接、和無形成本等在經濟上的負擔,可透過過疾病成本的研究來進行估算。[210]直接成本是對患病率和發病率研究來估算,而間接成本是通過人力資本方法、人口學方法、和摩擦成本(friction cost)方法估算的。[209] 但是,由於使用方法、與酒精消費有關的成本項目、和衡量技術的差異,經濟影響很難準確地被衡量。
酒精依賴對健康結果有深遠的影響。2016年在德國進行的一項研究發現,有酒精依賴問題的人產生的經濟負擔比沒有的人高出 50%。[211]在這項研究中,一半以上的經濟成本是由於生產力損失所造成,而只有 6%是由於對酒精問題做治療所致。這種經濟成本主要由30至49歲之間的人來承擔。在另一項根據來自8個歐洲國家的數據所做的研究中,[212]77%的酒精依賴患者患有精神病和軀體合併症(somatic comorbidity),從而增加醫療衛生和經濟上的成本。飲酒還會影響免疫系統,並在罹患愛滋病、肺炎、和結核病的人身上引起併發症。[213]
因酒精依賴而產生的間接成本非常巨大。最大的間接成本來自生產力損失,其次是過早死亡。[214]在美國,酒精依賴的男性勞動力參與率降低2.5%,收入的降低達到5.0%,缺勤率增加 0.5-1.2天。女性酗酒者的缺勤率則增加0.4-0.9天。過早死亡是酒精依賴間接成本的另一個重要因素。[215]在2004年,全球死亡人數中有3.8%與酒精有關(男性為6.3%,女性為1.1%)。60歲以下的人在全球因酒精導致的死亡人數中,比率更高,為5.3%。
一般而言,間接成本,例如因酒精依賴而導致的過早死亡,由於曠工曠職所引起,和導致出工者的生產力下降、財產損失、和執法成本,都遠遠超過直接醫療衛生和執法成本。[216] 匯總來自各方面所有的經濟成本,其影響可能佔一個國家國內生產總值(GDP)的0.45%至5.44%。[217]估計數字差距大的原因是由於對經濟負擔的衡量方法不一致,因為有些研究人員將長期飲酒可能帶來的正面影響,列入衡量之中[217][218][219]。
參見
參考文獻
註解
外部連結
Wikiwand - on
Seamless Wikipedia browsing. On steroids.

