Loading AI tools
Medical condition From Wikipedia, the free encyclopedia
Sporotrichosis, also known as rose handler's disease,[2] is a fungal infection that may be localised to skin, lungs, bone and joint, or become systemic.[2][4] It presents with firm painless nodules that later ulcerate.[3] Following initial exposure to Sporothrix schenckii, the disease typically progresses over a period of a week to several months.[1] Serious complications may develop in people who have a weakened immune system.[1]
| Sporotrichosis | |
|---|---|
| Other names | Rose thorn disease, rose gardener's disease,[1] rose handler's disease[2] |
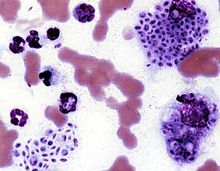 | |
| Cytologic preparation from a case of feline sporotrichosis; phagocytic cells show numerous variably-shaped yeast forms within | |
| Specialty | Infectious disease |
| Symptoms | Firm painless nodules that later ulcerate.[3] |
| Causes | Sporothrix schenckii[1] |
| Diagnostic method | |
| Differential diagnosis | Leishmaniasis, nocardiosis, mycobacterium marinum,[3] cat-scratch disease, syphilis, leprosy, sarcoidosis, tuberculosis[1] |
| Treatment | Antifungals, surgery[1] |
| Medication | Itraconazole, posaconazole, amphotericin B[1] |
| Prognosis | Good with treatment, poor if widespread disease[1] |
Sporotrichosis is caused by fungi of the S. schenckii species complex.[5][6] Because S. schenckii is naturally found in soil, hay, sphagnum moss, and plants, it most often affects farmers, gardeners, and agricultural workers.[7] It enters through small cuts in the skin to cause a fungal infection.[1] In cases of sporotrichosis affecting the lungs, the fungal spores enter by inhalation.[1] Sporotrichosis can be acquired by handling cats with the disease; it is an occupational hazard for veterinarians.[1]
Treatment depends on the site and extent of infection.[1] Topical antifungals may be applied to skin lesions.[1] Deep infection in the lungs may require surgery.[1] Systemic medications used include Itraconazole, posaconazole and amphotericin B.[1] With treatment, most people will recover,[1] but an immunocompromised status and systemic infection carry a worse prognosis.[1]
S. schenkii, the causal fungus, is found worldwide.[1] The species was named for Benjamin Schenck, a medical student who, in 1896, was the first to isolate it from a human specimen.[8]
Sporotrichosis has been reported in cats,[1] mules, dogs, mice and rats.[3]

Open sporotrichosis lesions on the skin will on occasion become superinfected with bacteria.[9] Cellulitis may also occur.[9]

Sporotrichosis is an acute infection with slow progression and often subtle symptoms. It is often difficult to diagnose, as many other diseases share similar symptoms and therefore must be ruled out.[citation needed]
Patients with sporotrichosis will have antibodies against the fungus S. schenckii; however, due to variability in sensitivity and specificity, antibody detection may not be a reliable diagnostic test for this disease. The confirming diagnosis remains culturing the fungus from the skin, sputum, synovial fluid, and cerebrospinal fluid. Smears should be taken from any draining fistulas or ulcers.[citation needed]
Cats with sporotrichosis are unique in that the exudate from their lesions may contain numerous infectious organisms. This makes cytological evaluation of exudate a valuable diagnostic tool in this species. Exudate is pyogranulomatous, and phagocytic cells may be packed with yeast forms. These yeast cells are variable in size; many are cigar-shaped.[citation needed]
Differential diagnoses includes: leishmaniasis, nocardiosis, mycobacterium marinum,[3] cat-scratch disease, leprosy, syphilis, sarcoidosis and tuberculosis.[1]
The majority of sporotrichosis cases occur when the fungus is introduced through a cut or puncture in the skin while handling vegetation containing the fungal spores. Prevention of this disease includes wearing long sleeves and gloves while working with soil, hay bales, rose bushes, pine seedlings, and sphagnum moss.
The risk of sporotrichosis in cats is increased in male cats that roam outdoors.[10] Accordingly, the risk may be reduced by keeping cats indoors or neutering them.[11] Isolating infected animals can also be a preventive measure.[11][12] The risk of spread from infected cats to humans can be reduced by appropriate biosafety measures, including wearing personal protective equipment when handling a cat with suspected sporotrichosis and by washing hands, arms and clothing after handling the cat.[12]
Treatment of sporotrichosis depends on the severity and location of the disease. The following are treatment options for this condition:[13]
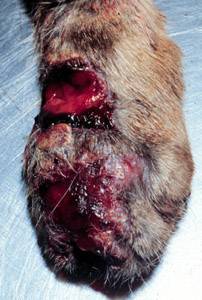
Sporotrichosis can be diagnosed in domestic and wild mammals. In veterinary medicine it is most frequently seen in cats and horses. Cats have a particularly severe form of cutaneous sporotrichosis. Infected cats may exhibit abscesses, cellulitis, or draining wounds that fail to respond to antibiotic treatment.[10]
Sporotrichosis can spread from nonhuman animals to humans (zoonosis). Infected cats in particular exude large quantities of Sporothrix organisms from their skin leasions and can spread the infection to people who handle them.[10][18] Although cats are the most common animal source, the infection has also been known to spread to humans from dogs, rats, squirrels, and armadillos.[19]
Seamless Wikipedia browsing. On steroids.
Every time you click a link to Wikipedia, Wiktionary or Wikiquote in your browser's search results, it will show the modern Wikiwand interface.
Wikiwand extension is a five stars, simple, with minimum permission required to keep your browsing private, safe and transparent.