Loading AI tools
Cancer screening involves efforts to detect cancer before symptoms appear.[1] This may involve blood tests, urine tests, other tests, or medical imaging.[1] The benefits of screening in terms of cancer prevention, early detection and subsequent treatment must be weighed against any harms.
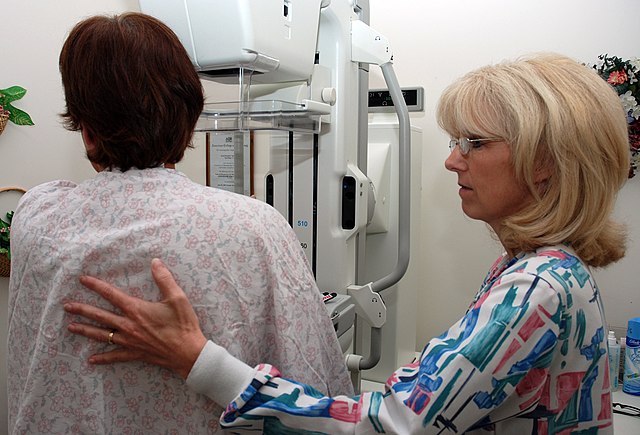
Universal screening or mass screening involves screening everyone, usually within a specific age group.[2] Selective screening identifies people who are known to be at higher risk of developing cancer, such as people with a family history of cancer.[2]
Screening can lead to false positive results and subsequent invasive procedures.[3] Screening can also lead to false negative results. Controversy arises when it is not clear if the benefits of screening outweigh the risks of the screening procedure, follow-up diagnostic tests and cancer treatments.
Screening tests must be effective, safe, well-tolerated with acceptably low rates of false positive and false negative results. If signs of cancer are detected, more definitive and invasive follow-up tests are performed to reach a diagnosis. Screening for cancer can lead to cancer prevention and earlier diagnosis. Early diagnosis may lead to higher rates of successful treatment and extended life. However, it may also falsely appear to increase the time to death through lead time bias or length time bias.
The following criteria are used by the UK National Screening Committee for making decisions about the effectiveness, acceptability and appropriateness of a screening test.[4]
The Condition
- The condition should be an important health problem
- The epidemiology and natural history of the condition, including development from latent to declared disease, should be adequately understood and there should be a detectable risk factor, disease marker, latent period or early symptomatic stage
- All the cost-effective primary prevention interventions should have been implemented as far as practicable
- If the carriers of a mutation are identified as a result of screening the natural history of people with this status should be understood, including the psychological implications
The Test
- There should be a simple, safe, precise and validated screening test
- The distribution of test values in the target population should be known and a suitable cut-off level defined and agreed
- The test should be acceptable to the population
- There should be an agreed policy on the further diagnostic investigation of individuals with a positive test result and on the choices available to those individuals
- If the test is for mutations the criteria used to select the subset of mutations to be covered by screening, if all possible mutations are not being tested, should be clearly set out
The Treatment
- There should be an effective treatment or intervention for patients identified through early detection, with evidence of early treatment leading to better outcomes than late treatment
- There should be agreed evidence based policies covering which individuals should be offered treatment and the appropriate treatment to be offered
- Clinical management of the condition and patient outcomes should be optimised in all health care providers prior to participation in a screening programme
The Screening programme
- There should be evidence from high quality Randomised Controlled Trials that the screening programme is effective in reducing mortality or morbidity
- Where screening is aimed solely at providing information to allow the person being screened to make an "informed choice" (eg. Down's syndrome, cystic fibrosis carrier screening), there must be evidence from high quality trials that the test accurately measures risk
- The information that is provided about the test and its outcome must be of value and readily understood by the individual being screened
- There should be evidence that the complete screening programme (test, *diagnostic procedures, treatment/ intervention) is clinically, socially and ethically acceptable to health professionals and the public
- The benefit from the screening programme should outweigh the physical and psychological harm (caused by the test, diagnostic procedures and treatment)
- The opportunity cost of the screening programme (including testing, diagnosis and treatment, administration, training and quality assurance) ) should be economically balanced in relation to expenditure on medical care as a whole (ie. value for money)
- There should be a plan for managing and monitoring the screening programme and an agreed set of quality assurance standards
- Adequate staffing and facilities for testing, diagnosis, treatment and programme management should be available prior to the commencement of the screening programme
- All other options for managing the condition should have been considered (e.g. improving treatment, providing other services), to ensure that no more cost effective intervention could be introduced or current interventions increased within the resources available
- Evidence-based information, explaining the consequences of testing, investigation and treatment, should be made available to potential participants to assist them in making an informed choice
- Public pressure for widening the eligibility criteria for reducing the screening interval, and for increasing the sensitivity of the testing process, should be anticipated
- Decisions about these parameters should be scientifically justifiable to the public
- The likelihood of the test correctly identifying cancer: If the test is not sensitive, then it may miss cancers. If the test is not specific, then it may wrongly indicate cancer in a healthy person. All cancer screening tests produce both false positives and false negatives, and most produce more false positives. Experts consider the rate of errors when making recommendations about which test, if any, to use. A test may work better in some populations than others. The positive predictive value is a calculation of the likelihood that a positive test result actually represents cancer in a given individual, based on the results of people with similar risk factors.
- Possible harms from the screening test itself: Some types of screening tests are potentially harmful to the human body. There is a very small chance, for example, that the x-rays used in mammography could cause cancer in a healthy person.
- Possible harms from follow-up procedures: If the screening test is positive, further diagnostic testing is normally done, such as a biopsy of the tissue. If the test produces many false positives, then many people will undergo needless medical procedures, some of which may be dangerous.
Breast cancer
There is general agreement in the scientific community that breast screening reduces mortality from the disease.[5]
There is some controversy however about the number of lives saved by breast screening and the number of cancers diagnosed that would not have caused any health problems in the participants' lifetime.[6]
Similarly, for breast cancer, there have recently been criticisms that breast screening programs in some countries cause more problems than they solve. This is because screening of women in the general population will result in a large number of women with false positive results which require extensive follow-up investigations to exclude cancer, leading to having a high number-to-treat (or number-to-screen) to prevent or catch a single case of breast cancer early.
The U.S. Preventive Services Task Force (USPSTF) recommends screening mammography once for every two years for all women aged 50—74, with decisions about screening younger and older women being determined by consideration of the individual's risk factors and the benefits and harms of screening. They do not recommend either breast self-examination or clinical breast examination.[7] Their recommendation is similar to the World Health Organization's, and less aggressive than most North American organizations. A 2009 Cochrane review came to slightly different conclusions with respect to breast cancer screening stating that routine mammography may do more harm than good.[8]
Cervical cancer

Cervical cancer screening via the Pap smear has the best cost-benefit profile of all the forms of cancer screening from a public health perspective as, being largely caused by a virus, it has clear risk factors (sexual contact), and the natural progression of cervical cancer is that it normally spreads slowly over a number of years therefore giving more time for the screening program to catch it early. Moreover, the test itself is easy to perform and relatively cheap.
The U.S. Preventive Services Task Force (USPSTF) strongly recommends cervical cancer screening in American women who are sexually active and have a cervix at least until the age of 65, usually every three years.[9] Their recommendation is typical of professional organizations and other government agencies in the US and Canada.
Bowel cancer

The US Preventive Services Task Force recommends screening for bowel cancer using fecal occult blood testing, sigmoidoscopy, or colonoscopy, in adults, beginning at age 50 years and continuing until age 75 years.[10]
Prostate cancer
When screening for prostate cancer, the PSA test may detect small cancers that would never become life threatening, but once detected will lead to treatment. This situation, called overdiagnosis, puts men at risk for complications from unnecessary treatment such as surgery or radiation. Follow up procedures used to diagnose prostate cancer (prostate biopsy) may cause side effects, including bleeding and infection. Prostate cancer treatment may cause incontinence (inability to control urine flow) and erectile dysfunction (erections inadequate for intercourse).[citation needed]
Lung Cancer
According to the U.S. Preventive Services Task Force (USPSTF), there is insufficient evidence to recommend for or against screening for lung cancer.[11]
Recent research suggests that screening heavy smokers may be effective.
There is insufficient evidence to recommend for or against screening for skin cancer,[12] and oral cancer.[13] Routine screening is not recommended for bladder cancer,[14] testicular cancer,[15] ovarian cancer,[16] and pancreatic cancer.[17]
According to the U.S. Preventive Services Task Force (USPSTF), there is insufficient evidence to recommend for or against screening for prostate cancer in men under 75.[18] Routine screening is not recommended for prostate cancer in men over 75.[18] Most North American medical groups recommend individualized decisions about screening, taking into consideration the risks, benefits, and the patients' personal preferences.
Use of medical imaging to search for cancer in people without clear symptoms is similarly marred with problems. There is a significant risk of detection of what has been recently called an incidentaloma - a benign lesion that may be interpreted as a malignancy and be subjected to potentially dangerous investigations.
Wikiwand in your browser!
Seamless Wikipedia browsing. On steroids.
Every time you click a link to Wikipedia, Wiktionary or Wikiquote in your browser's search results, it will show the modern Wikiwand interface.
Wikiwand extension is a five stars, simple, with minimum permission required to keep your browsing private, safe and transparent.