Loading AI tools
 | This is a user sandbox of Emb47. You can use it for testing or practicing edits. This is not the sandbox where you should draft your assigned article for a dashboard.wikiedu.org course. To find the right sandbox for your assignment, visit your Dashboard course page and follow the Sandbox Draft link for your assigned article in the My Articles section. |
The transmission and epidemiology of Scarlet Fever is are dependent on those of Group A Streptococcal Pharyngitis since the majority of cases are derived from that pharyngeal infection. It occurs equally in both males and females.[1] Children are most commonly infected, typically between 5-15 years old. Although streptococcal infections can happen at any time of year, infection rates peak in the winter and spring months, typically in colder climates.[2] Transmission occurs between humans in close contact, via respiratory droplets (for example, saliva or nasal discharge.[2] A person in close contact with another person infected with Group A Streptococcal Pharyngitis has a 35% of becoming infected.[3] 1 in 10 children who are infected with Group A Streptococcal Pharyngitis will develop Scarlet Fever.[1]
The amount of scarlet fever cases has decreased over time along with the morbidity and mortality caused by the disease. The improvement in prognosis can be attributed to the use of penicillin in the treatment of this disease.[4] The cause for the change in overall frequency of the disease however is unclear as strains of group A streptococci that are capable of causing scarlet fever are still present.[5]
- Typical symptoms of streptococcal pharyngitis (inflamed throat, also known as strep throat) [4]
- Sore throat, painful swallowing
- Fever - typically over 39°C (102.2°F)
- Fatigue
- Enlarged and reddened tonsils with yellow or white exudates present (this is typically an exudative pharyngitis)[6]
- Enlarged and tender lymph nodes usually located on the front of the neck[1]
- Rash which has a characteristic appearance, spreading pattern, and desquamating process (described below)
- "Strawberry tongue"
- The tongue starts out by having a white coating on it while the papillae of the tongue are swollen and reddened. The protrusion of the red papillae through the white coating gives the tongue a "white strawberry" appearance.
- Then a few days later (following the desquamating process, or the shedding of the tissue that created the white coating) the whiteness disappears while the red and enlarged papillae give it the "red strawberry" appearance. [7]
- Note that this involvement of the tongue is a part of the rash that is characteristic of scarlet fever. [8]
- Pastia's Lines[9]
- Lines of petechiae that appear as pink/red areas located in arm pits and elbow pits
- Vomiting and abdominal pain[4]
Note that the following signs and symptoms will usually be absent:[4]
(The presence of these symptoms indicates that the illness is more likely due to a virus rather than a bacterial infection)
- Cough
- Hoarseness
- Runny nose
- Diarrhea
- Conjunctivitis
Rash:
The rash begins 1-2 days following the onset of symptoms caused by the strep pharyngitis (sore throat, fever, fatigue).[2] This characteristic rash has been denoted as "scarlatiniform" and it appears as a diffuse redness of the skin with small papules, or bumps, that resemble goose pimples.[7][5] These bumps are what give the characteristic sand paper texture to the rash. The reddened skin will blanch when you apply pressure to it. It is possible for the skin to be itchy however it will not be painful.[7] It usually first appears on the trunk and then gradually spreads out to the arms and legs. [5] The palms, soles and face are usually left uninvolved by the rash. The face is however is usually flushed, most prominent in cheeks, with a ring of paleness around the mouth.[10] After the rash spreads, it becomes more pronounced in creases in the skin, such as the skin folds in the inguinal and axillary regions of the body.[9] Also in those areas it is possible for there to be Pastia’s Lines which are petechiae arranged in a linear pattern.[9] Within 1 week of onset the rash beings to fade followed by a longer process of desquamation, or shedding of the outer layer of skin, that lasts several weeks.[1] The desquamation process usually begins on the face and progresses downward on the body.[7] After the desquamation the skin will be left with a sunburned appearance.[2]
Mouth:
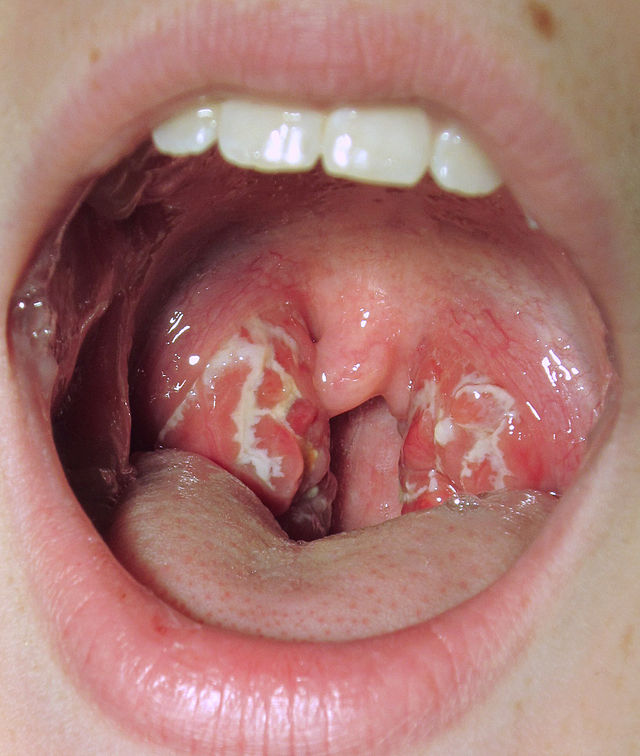
The streptococcal pharyngitis that is the usual presentation of scarlet fever in combination with the characteristic rash commonly involves the tonsils. The tonsils will appear swollen and reddened. The palate and uvula are also commonly affected by the infection. The involvement of the soft palate can be seen as tiny red and round spots known as Forscheimer spots. [6]
Variable presentations:
The clinical features of scarlet fever can differ depending on the age and race of the person. Children less than 5 years old can have atypical presentations. Children less than 3 years old can present with nasal congestion and lower grade fever than older children.[3] Infants can potentially only present with increased irritability and decreased appetite.[3]
Children who have darker skin can have a different clinical presentation in that the redness of the skin involved in the rash and the ring of paleness around the mouth can be less obvious or visible.[7] Clinical suspicion based off accompanying symptoms and diagnostic studies are important in these cases.
Course:
After the Streptococcal infection is transmitted to the individual, it takes between 12 hours to 7 days for the infection to cause the abrupt onset of the first clinical signs of Strep Pharyngitis including fever, fatigue, and sore throat. The characteristic scarlatiniform rash then comes 12-48 hours later. During the first few days of the rash development and rapid generalization, the Pastia's Lines and strawberry tongue will also present.[7] The rash starts fading within 3-4 days followed by the desquamation of the rash that will last several weeks to a month.[2][6]. If the case of scarlet fever is uncomplicated, recovery forth fever and clinical symptoms other than than the process of desquamation occurs in 5-10 days.[11]
The complications that can arise from scarlet fever when left untreated or inadequately treated can be divided into two categories: suppurative and nonsuppurative.
Suppurative complications: These are rare complications that either arise from direct spread to structures that are close to the primary site of infection, which in most cases of Scarlet Fever is the pharynx. Possible problems from this method of spread include peritonsillar or retropharyngeal abscesses, cellulitis, mastoiditis or sinusitis. It is also possible for the streptococcal infection to spread through the lymphatic system or the blood to areas of the body further away from the pharynx. A few examples of the many complications that can arise from those methods of spread include endocarditis, pneumonia, or meningitis.[10]
Nonsuppurative complications: These complications arise from certain subtypes of the group A streptococci that cause an autoimmune response in the body through what has been termed molecular mimicry. The antibodies that the person’s immune system developed to attack the Group A Streptococci are in these cases also able to attack the person's own tissues. The following complications result depending on which tissues in the person's body are targeted by those antibodies. [5]
- Acute Rheumatic Fever: This is a complication that results 2-6 weeks after a Group A Streptococcal infection of the upper respiratory tract.[2] It presents in developing countries, where antibiotic treatment of streptococcal infections is less common, as a febrile illness with several clinical manifestations that are organized into what is called the Jones criteria. These criteria include arthritis, carditis, neurological issues and skin findings. There also needs to be evidence of a prior Group A Streptococcal infection in the upper respiratory tract (as seen in Streptococcal Pharyngitis and Scarlet Fever). The carditis is the result of the immunologic response targeting the person's heart tissue and it is the most serious sequelae that develops from acute rheumatic fever. When this involvement of the heart tissue occurs it is called Rheumatic Heart Disease. In most cases of Rheumatic Heart Disease, the mitral valve is affected, ultimately leading to mitral stenosis. [3]
- Poststreptococcal Glomerulonephritis: This is inflammation of the kidney that presents 1-2 weeks after a Group A Streptococcal Pharyngitis. It can also develop after an episode of Impetigo or any Group A streptococcal infection in the skin.[2] It is the result of the autoimmune response to the streptococcal infection impacting the part of the kidney. Patient’s present with what is called acute nephritic syndrome in which they have high blood pressure, swelling and urinary abnormalities. Urinary abnormalities include blood and protein found in the urine as well as less urine production overall.[2]
- Poststreptococcal reactive arthritis: The presentation of arthritis after a recent episode of group A streptococcal pharyngitis raises suspicion for acute rheumatic fever since it is one of the Jones criteria for that separate complication. However, when the arthritis is an isolated symptom then it is referred to as poststreptococcal reactive arthritis. This arthritis can involve a variety of joints throughout the body, unlike the arthritis of acute rheumatic fever which primarily impacts larger joints like the knee joints. It can present less than 10 days after the group A streptococcal pharyngitis.[2]
The rash of Scarlet Fever, which is what differentiates this disease from an isolated Group A Strep pharyngitis (or strep throat), is caused by specific strains of Group A Streptococcus that produce a pyrogenic exotoxin.[2] These toxin producing strains cause scarlet fever in people who do not already have antitoxin antibodies. Streptococcal Pyrogenic Exotoxins A, B, and C (speA, speB, and speC) have been identified. The pyrogenic exotoxins are also called erythrogenic toxins and cause the erythematous rash of Scarlet Fever.[2] The strains of Group A Streptococcus that cause Scarlet Fever need specific bacteriophages in order for there to be pyrogenic exotoxin production. Specifically, Bacteriophage T12 is responsible for the production of speA.[12]
Streptococcal Pyrogenic Exotoxin A, speA, is the one that is most commonly associated with cases of Scarlet Fever that are complicated by the immune mediated sequelae Acute Rheumatic Fever and Poststreptococcal Glomerulonephritis.[6]
These toxins are also known as “superantigens” because they are able to cause an extensive immune response within the body through activation of some of the main cells responsible for the persons immune system.[11] The body responds to these toxins by making antibodies to those specific toxins. However, those antibodies do not completely protect the person from future Group A Streptococcal infections since there are 12 different pyrogenic exotoxins possible.[2]
Although the classic presentation of Scarlet Fever can be clinically diagnosed, a large amount of variation and severity of presentation exist so further testing is required to distinguish it from other illnesses.[7] Also, history of a recent exposure to someone with a Group A Strep Pharyngitis can aid in a clinical diagnosis.[2] There are two microbiologic tests used to confirm clinical suspicion of scarlet fever.[3]
- Rapid Antigen Detection Test
- Throat Culture
The Rapid Antigen Detection Test is a very specific test but not very sensitive. This means that if the result is positive (indicating that the Group A Strep Antigen was detected and therefore confirming that the patient has a Group A Strep Pharyngitis) then it is appropriate to treat them with antibiotics. However, if the Rapid Antigen Detection Test is negative (indicating that they do not have Group A Strep Pharyngitis), then a throat culture is required to confirm since it could be a false negative result.[13] The throat culture is the current gold standard for diagnosis.[3]
Choosing whether or not to test a patient for Strep Throat when they present with a sore throat is a common choice faced in many primary care doctor's offices and emergency rooms. A list of criteria, called the Centor criteria were created to make this decision easier and to reduce the amount of unnecessary testing done.
Serologic testing looks for the antibodies that the body produces against the streptococcal infection including antistreptolysin-O and antideoxyribonuclease B. It takes the body 2-3 weeks to make these antibodies so this type of testing is not useful for diagnosing a current infection. However, it is useful when assessing a patient who may have one of the complications from a previous streptococcal infection.[1][3]
Differential Diagnosis:
- Viral Exanthem: Viral infections are often accompanied by a rash that can be described as morbilliform or maculopapular. This type of rash is accompanied by a prodromal period of cough and runny nose in addition to a fever, indicative of a viral process.[5]
- Allergic or Contact Dermatitis: The erythematous appearance of the skin will be in a more localized distribution rather than the diffuse and generalized rash seen in Scarlet Fever. [1]
- Drug Eruptions: These are potential side effects of taking certain drugs such as Penicillin. The reddened maculopapular rash that results can be itchy and be accompanied by a fever.[14]
- Kawasaki Disease: Children with this disease also present with a strawberry tongue and undergo a desquamative process on their palms and soles. However these children tend to be younger than 5 years old, their fever lasts longer (at least five days) and they have additional clinical criteria (including signs such as conjunctival redness and cracked lips) that can help distinguish this from Scarlet Fever. [15]
- Toxic Shock Syndrome: Both Streptococcal and Staphylococcal bacteria can cause this syndrome. Clinical manifestations include diffuse rash and desquamation of the palms and soles. Can be distinguished from Scarlet Fever by low blood pressure, the rash will lack sandpaper texture, and multi-organ system involvement.[16]
- Staphylococcal Scalded Skin Syndrome: This is a disease that occurs primarily in young children due to a toxin producing strain of the bacteria Staphylococcus Aureus. The abrupt start of the fever and diffused sunburned appearance of the rash can resemble Scarlet Fever. However, this rash is associated with tenderness and large blister formation. These blisters easily pop and then cause the skin to peel.[17]
- Staphylococcal Scarlet Fever: The rash is identical to the streptococcal scarlet fever in distribution and texture however the skin affected by the rash will be tender.[7]
Wikiwand in your browser!
Seamless Wikipedia browsing. On steroids.
Every time you click a link to Wikipedia, Wiktionary or Wikiquote in your browser's search results, it will show the modern Wikiwand interface.
Wikiwand extension is a five stars, simple, with minimum permission required to keep your browsing private, safe and transparent.